Kyrenia IVF / ICSI Treatment
What is ICSI?
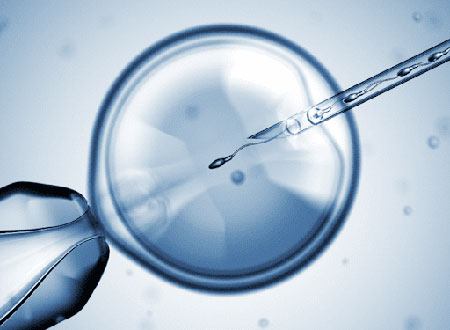
ICSI is a special technique in which a single sperm is injected into the center of the egg after the egg is retrieved. The technique is commonly used when the sperm count or motility is low (ability to swim towards the egg). ICSI is also preferred for several reasons, for example in conjunction with pre-implantation genetic diagnosis (PGD) or when sperm DNA fragmentation is high.
How is ICSI Done?
Intracytoplasmic sperm injection (ICSI) involves the direct injection of sperm into eggs obtained from the female partner.
In the lab, embryologists will inject a single sperm into each egg.
There are five simple steps for ICSI:
After the females' egg competition, the mature egg is held with a special pipette.
A single sperm is injected into the mature egg.
The needle is then carefully inserted through the shell of the egg and into the cytoplasm of the egg.
Sperm are injected into the cytoplasm.
The eggs are checked over the next 24 hours for normal fertilization.
Once ICSI is complete and fertilization is successful it will develop into an embryo, the embryo transfer procedure is to place the embryo in the woman's uterus.
How long does it take for embryos to develop?
The day after sperm is injected into each egg, embryologists will look for signs of fertilization. The next day they check that the embryo has broken down. Embryos can be transferred at any stage from day 3 to day 6. If day 3 embryos wait for day 5 embryos it will be a 6 or 8 cell embryo, the embryos should reach a blastocyst stage.
Embryologists monitor and grade embryos very carefully. In most cases, if the embryos are well developed, they do not recommend transferring more than 2 embryos to reduce the risk of multiple pregnancy.
Untransferred embryos?
If you have left behind quality embryos that were not transferred on the day of transfer, they can be frozen. Frozen embryos can be stored for a long time for future transfers.
Is ICSI for me?
ICSI may be recommended when there is reason to suspect that fertilization may be difficult to achieve. ICSI is often used with couples dealing with male infertility factors. Male infertility factors can include any of the following: low sperm count, poor motility or motility of the sperm, poor sperm quality, sperm incapable of penetrating an egg, or azoospermia.
Azoospermia is a condition in which there is no sperm in a man's ejaculate. There are two types of azoospermia: obstructive and non-obstructive.
We may recommend ICSI in the following situations:
Male partner's sperm count is very low
The male partner's sperm have problems such as poor motility (not moving normally) or poor morphology (abnormal shape).
Previous attempts at reconciliation have failed
Sperm must be surgically collected from the man's testicles or epididymis, for example if a vasectomy has been performed
You use frozen sperm in your treatment
You are performing a pre-implantation genetic diagnosis or screening